Abstract
Renal cell carcinoma (RCC) metastasis to the parotid region is extremely rare. Diagnosis can only be made histopathologically. A 74-year old female presented at our clinic with complaints of swelling in the left parotid region. The patient had no other systemic complaint, so after radiological examination and fine needle aspiration, superficial parotidectomy was applied. As histopathological examination results showed RCC, abdominal computed tomography (CT) was taken and a mass was determined in the left kidney. The clinical, radiological and histopathological results of this rare case are presented in this paper.
Introduction
Metastasis to the parotid gland is rarely seen [1]. Metastases often originate in the head and neck and the majority are squamous cell carcinoma and malignant melanoma [1]. Infraclavicular-originated metastasis is extremely rare (0.16%-4%) [1]. RCC has a high tendency to early metastasis, but metastasis in the head and neck region is extremely rare [2]. The case is here presented of a 74-year old female patient with parotid metastasis of renal cell carcinoma.
Case Report
A 74-year old female patient presented at our clinic with a painless mass in the left parotid region which had been there for some time. The patient had no genitourinary complaints and the laboratory test results were normal. A mobile mass 3 x 2cm in size was determined in the left parotid region. Other ENT examination findings were normal. As a result of fine needle aspiration biopsy made under ultrasound (USG) guidance, a mass of hypercellular appearance was determined with most of the nuclei oval or round with eccentric positioning with a pleomorphic base and hyperchromatic nucleus which could not be discounted as a malignancy. On the neck CT image, a solid lesion was observed, 20 x 13mm in diameter located in the left parotid gland and superficial lobe with regular borders and evident lobulation showing mild contrast involvement. It was initially evaluated as pleomorphic adenoma.
During the operation, a mass was observed in the parotid superficial lobe, 5 x 2cm in size which did not show invasion into the surrounding tissue and left-side superficial parotidectomy was applied (Figure 1). No complication developed during surgery and the patient was discharged on postoperative Day 3.
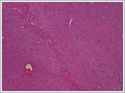
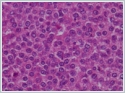
As a result of the postoperative pathology examination, a tumour was observed in the parotid tissue, formed of cells in a relatively monotone appearance with eosinophilic and clearcytoplasm, located in a diffuse pattern between the fine capillary vascular network showing infiltration to the surrounding fat tissue (Figures 2a, 2b).
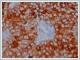
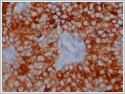
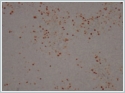
Tumour cells which were examined immunohistochemically showed positive staining with pancytokeratin, and diffuse and strong positivity with RCC (Figure 3a) and approximately 20% Ki67 proliferation was reported (Figure 3b). As a result of these findings, abdominal CT was taken which showed tumour findings in a kidney localisation consistent with RCC metastasis. However, the patient refused any further tests or treatment.
Discussion
Metastasis in the parotid gland is most frequently from malignant melanoma (45%) followed by squamous cell carcinoma (37%) in the head and neck region [3,4]. Metastasis of RCC in the parotid region is extremely rare. RCC has the features to be able to metastise to atypical tissue or organs but there are few reports of parotid metastasis in literature [5]. RCC constitutes 80%-85% of malignant tumours of the kidney. Clear cell carcinoma is histopathologically the most frequently seen subtype. As themajority of RCC show symptoms when the tumour has reached large dimensions, patients generally present at advanced stages of the disease. The most frequently determined findings are haematuria, abdominal pain and a palpable mass. However, these three symptoms to gether are seen in less than 10% of cases. RCC may be bilateral in 1%-3% of cases [6]. In the case presented here, the patient had no genitourinary symptoms and the preoperative full urine test result was normal. The most common locations of RCC metasasis are the lungs, bones, liver and brain. However, there may be metastasis in any organ or tissue such as the thyroid, parotid, pancreas, softtissue, or the musculo-skeletal system [6]. The most frequently determined primary tumour regions of clear cell renal carcinoma in autopsyseries are the breast and the lungs. In the current case, RCC metastasis was determined in the examination of the parotidectomy material.
The majority of RCC are seen over the age of 40 years and the peak is in the 7th decade [7]. The case presented here was a 74-year old female. The most frequently determined finding of parotid gland metastasis is a mass leading to pain and tension [8]. The current case presented with a painless swelling. It has been reported that the first finding of RCC could be parotid gland metastasis. RCC can metastise to the parotid gland through a hematogenous route [3]. In the current case, RCC was determined in the kidney after the mass was determined in the parotid gland. The etiology of RCC has not yet been fully clarified. However, hereditary factors are known to play a significant role. VHL gene mutation is the most commonly seen genetic anomaly [7]. From a biological aspect, RCC has the capability to metastise to atypical tissues or organs.
The parotid metastasis determined in the current case can be accepted as the normal course of RCC. In patients with a history of RCC, it must be kept in mind that metastasis can be observed in atypical localisations, not just the head and neck, and therefore further tests should be applied when metastasis is suspected.
References
- Vara A, Madrigal B, Pérez del Río MJ. Parotid metastasis from renal clear cell adenocarcinoma. An unusual site for metastasis. Urol Int. 1998;61:196–198.
- Leibovich BC, Pantuck AJ, Bui MH. Current staging of renal cell carcinoma. Urol Clin North Am. 2003;30:481–497.
- Spreafico R et al. Parotid metastasis from renal cell carcinoma: a case report and review of the literature. Actaotorhinolaryngologica Italica. 2008;28(5):266–268.
- Barnes L. Metastases of the head and neck: An overview. Head Neck pathol.2009;3:217-224
- Park YW, Hlivko TJ. Parotid gland metastasis from renal cell carcinoma. The Laryngoscope. 2002;112(3):453–455.
- Mrena R et al. Histopathological findings in parotid gland metastases from renal cell carcinoma. European Archives of Oto-Rhino-Laryngology. 2008;265(9):1005–1009.
- Alpers CE. The kidney. In Kumar V,Abbas AK, Fauston, editors. Robbins and Cotran.Pathologic Basis of Disease. Philadelphia:Elsevier;2010:905-981
- Li L et al. Metachronous bilateral-metastases of renal cell carcinoma to the parotid gland. J oral maxillofac surg.2001;59:434-438.
|