|
|||||
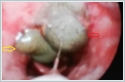
AbstractLeeches are blood-sucking hermaphrodite parasites and more common in rural areas. They usually occur after drinking untreated rural water or swimming in rivers or lakes. In this way, it mostly involves the upper respiratory tract. In this case, we presented a 65-year-old female patient who presented with hemoptysis due to the leech in the oropharynx.IntroductionLeeches,blood-sucking hermaphrodite parasites, are classified in the phylum Annelida of the Hirudinea class. Leech infections usually occur with aquatic leeches and are more common in rural areas of Asia, Mediterranean region and Africa [1]. The most common leech species in humans are Hirudo medicinalis and Limnatis nilotica. Limnatis nilotica is also the most common leech reported in our country [2]. Leech infection is a very rare condition in humans, it mostly occurs after drinking untreated rural water or swimming in rivers or lakes. It can be localized anywhere in humans including the upper respiratory and digestive tract, nose, pharynx, esophagus and rarely the larynx [3]. It can also hold onto the mucous membranes such as conjunctiva, trachea, bronchus, vagina and rectum [4]. Therefore, the patient's complaints may vary according to the localization of the leech. Case ReportA 65-year-old female patient applied to our otolaryngology clinic with complaints of bleeding from the mouth and painful swallowing. It was learned from the story of the patient that her complaints had been for a month and that she had previously applied to another health institution with these complaints. On the oropharynx examination of the patient, a dark gray colored body was observed in the oropharynx, posterior to the uvula. In the nasopharyngoscopy performed to identify the mass more clearly, a leech with a size of 2x4 cm attached to the oropharynx was seen (Figure 1).
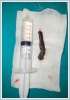
Nasopharyngeal angiofibroma, anthracoanal polyp and malignant tumors could be considered in the differential diagnosis in terms of the location of the mass. However, we did not perform any radiological examination for these differential diagnoses. Because the tail movements of the leech were clearly visible. Therefore, it was understood that this was an organism coming from outside of the body. It was detected that the leech advances its tail towards the larynx and withdraws it. The patient also stated that she lived in rural areas and sometimes drank water from water sources such as rivers. Since leech was seen limited from the oropharynx, we decided to take the patient into operation under general anesthesia. In the laboratory examination of the patient, the hemoglobin level was 14.8 g/d Land the white blood cell count was 10.65 10[˄]3/mL. Other blood parameters were unremarkable. Intraoperatively, after the application of automatic mouth retractor, the uvula was removed and the leech was totally removed with forceps (Figure 2).
Subsequent minimal bleeding was controlled with local tampons. In the postoperative period, patient did not develop any complications and discharged with recommendations. DiscussionAlthough the transmission of leeches to humans is usually cutaneous, they can also occur due to swimming in infected waters or drinking these waters. For this reason, many cases have been reported from less developed countries where safe water use is a major problem [1,5]. Leeches can cause symptoms such as nasal congestion, dyspnea, dysphagia, dysphonia, hemoptysis, hematemesis, bleeding or a globus sensation when they attach to the upper respiratory and digestive system. Leeches generally do not carry diseases, but they can cause infection in 4-20 % of patients due to symbiotic livings creatures in their intestinal system [1-3,6]. Leech saliva contains a number of compounds that help it nourish itself. While leeches feed, they secrete hirudin. This secretion causes mucosal bleeding. Histamine-like substances, another salivary component, also inhibit capillary vasoconstriction and cause mucosal bleeding. The purpose of these secretory substances is to keep the leech attached to the host's vascular system for a longer period of time and to ensure that the leech feeds longer. Leeches can suck up to 80-90 % of their average weight or 150 cc of blood in 48 hours. In some cases, this can cause severe anemia [5,7]. Ağın et al. [4] presented a case of pharyngeal leech in a 5-year-old child that caused severe anemia which required urgent blood transfusion. Cundal et al. [8] reported that three cases of their six pharyngeal leech (Myxobdella Africana) patients were severely anemic and one of them died. In our case, the patient did not have anemia and other blood parameters were normal, but the patient's complaints has started recently. Leeches adhere tightly to mucosal surfaces with their strong mouths, if the excision of leech becomes unsuccessful in the first move, they can adhere to the tissue more strong. It has been reported that injection of cocaine or lidocaine to the leech causes paralysis of the leech and this manipulation facilitates removal of the leech [1,2,9]. Koca et al. [7] suggested that the best method of removing leeches from the upper aerodigestive tract is to perform direct laryngoscopy under general anesthesia. It has been claimed that the administration of general anesthetic and myorelaxant drugs to the patient will cause to easily seperation of leech especially which located in the risky locations such as the pharynx and larynx to be easily [5]. In our case, we did not do any radiological imaging before the operation. Because it was understood that this organism was a leech due to the its active tail movements and its external appearance. In addition, diseases in differential diagnosis were also not considered as a priority. Because most of these diseases arise from the nasopharynx or paranasal sınuses, but our case did not extend to the nasopharynx. Before the operation, it was decided to perform the removal procedure under general anesthesia, as the patient could not adapt to the local examination and the tail of the leech was mobile and the tail was displaced towards the nasopharynx. Hence the leech was not always fully visible in the oropharynx. In order to avoid possible aspiration of leeches during intubation, the patient was intubated in the hyperextended position of the head. Another point to be considered during the removal of leech is the removal of the leech in one piece. Recurrent bleeding may occur in cases where the head with strong teeth is left behind [7]. Conclusion Although rarely, it should be kept in mind that leeches may occur anywhere in the upper respiratory tract of patients especially came from rural areas with complaint of epistaxis, sore throat, hemoptysis and globus sensation. References
|
|||||
| Keywords : Sülük , orofarinks , hemoptizi | |||||
|