|
|||
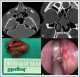
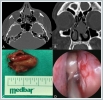
AbstractConcha bullosa is one of the most common anatomical variant of sinonasal area and is usually asymptomatic. Concha bullosa pyocele may occur when a mucocele becomes infected. The differential diagnosis of a massive mucocele or pyocele of the middle turbinate from other intranasal masses can be greatly faciliated by intranasal endoscophic examination and advanced radiographic techniques like computed tomography and magnetic resonance imaging. We report a case of massive concha bullosa pyocele which has caused nasal obstruction and headache for six months. The treatment of the patient was finalized by the endoscopic resection of lateral and inferior walls of the concha bullosa pyocele.IntroductionConcha bullosa, also known as the middle turbinate pneumatization, is often asymptomatic. However, as it is the most common variation of sinonasal anatomy, it should be considered in patients presenting with nasal obstruction, headache, and impaired smell function. The pathology of concha bullosa may widely vary from a mild mucosal edema to polyps, retention cyst, empyema, and fungal aggregates of the sinus [1]. Case ReportA 27-year-old male patient was admitted to our clinic with reduced nasal breathing and headache for six months. The patient had no history of epistaxis and allergic reactions. Anterior rhinoscopic and endoscopic examination revealed a mass lesion with a smooth surface which covered the left nasal cavity almost completely, originating from the anterior middle turbinate. Paranasal sinus computed tomography (CT) showed an 18x28 mm polypoid lesion of the anterior middle turbinate of the left nasal cavity with a soft tissue density. (Figure 1A-B) The septum was deviated to the right with normal adjacent sinus pneumatization. The mass was excised under general anesthesia. A dense purulent material within the mass was aspirated during excision. (Figure 1C-D) No postoperative complication was observed. The pathological examination result was reported as pyocele. The septum was deviated to the right with normal adjacent sinus pneumatization. The mass was excised under general anesthesia. A dense purulent material within the mass was aspirated during excision. (Figure 1C-D)
DiscussionAlthough the mechanism of concha bullosa is unclear, the possible pathogenesis can be explained by the “ex vacua” theory. As in our case, the middle turbinate can be pneumatizated which is located in the septal concave due to reduced air flow in the deviated side and increased air flow in the counterpart [2]. There is a number of studies showing a high concomitance rate of concha bullosa and septal deviation [3,4,5]. However, these studies have not established any association between the size of concha bullosa and complaints of patients [3]. Certain obstructions which interfere with drainage of concha bullosa may lead to mucocele development and an infected mucocele may lead to a pyocele of concha bullosa [6]. Inflammatory cells within pyocele may induce bone destruction and a giant pyocele may develop due to diminished bone support [7]. Concha bullosa is often asymptomatic and usually incidentally diagnosed. Depending on its size, patients may present with nasal obstruction, headache, and impaired smell function [8,9]. Whether it may cause sinus pathologies due to mass effect is still controversial. Stallman et al. [4] performed computed tomography on 1,095 patients with sinusitis and reported that the incidence of paranasal sinus inflammatory disease was 73% and 78% in patients with and without concha bullosa, respectively. The authors concluded that there was no significant difference in the development of sinusitis among the patients with and without concha bullosa. In our case, although we observed a mass lesion which covered the left nasal cavity almost completely, endoscopic and radiological examinations demonstrated no chronic infection sign in the adjacent sinuses. In addition, vascular lesions such as juvenile angiofibroma and hemangioma and intracranial lesions should be considered in the differential diagnosis. Therefore, the diagnosis should be based on clinical and endoscopic findings and be subsequently confirmed by imaging studies such as CT or magnetic resonance imaging (MRI). In our case, we detected a mass originating from the anterior middle turbinate through CT. Aspiration of the purulent material within the mass during surgery supported the diagnosis of pyocele. Furthermore, asymptomatic concha bullosa does not require treatment; however, concha bullosa cases which cause obstruction of the ostiomeatal complex and disease in the paranasal sinuses and those which cause airway obstruction should be surgically treated [10]. Subdural empyema and orbital complications due to the pyocele of concha bullosa have been reported in the literature [11]. Therefore, these cases should be always surgically treated. In our case, the mass located in the left anterior middle turbinate was surgically excised. Similar to other reported cases [2,8,9], partial excision of the pathological concha was sufficient in our case. In conclusion, although rare, the pyocele of concha bullosa should be considered in patients suffering from headache and nasal obstruction. Minimally invasive endoscopic techniques are useful in the treatment of this pathology which may cause severe intracranial and orbital complications. References
|
|||
| Keywords : Konka bülloza , Piyosel , Burun tıkanıklığı | |||
|