|
|||||||||
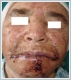
AbstractNodular hidradenoma, also known as clear cell hidradenoma or acrospiroma is an uncommon benign tumor of apocrine sweat glands. Most commonly it is seen in adult and female population. It usually presents as slowly enlarging, solitary nodule and occurs on the scalp, face, trunk, proximal region of the arms and legs. Our patient was a 77 year old female presenting with an unpainful and firm mass on her lower lip. In literature, there are only a few case of hidradenoma occurring on the lip. In this article, we presented a case of benign nodular hidradenoma localizated on the lower lip.IntroductionNodular hidradenoma is a rare tumor of sweat glands. It usually has ecrine differentiation, but it is known that hidradenomas have apocrine differentiation also [1-3]. These tumors present as solitary intradermal nodules, solid or cystic, slowly growing, firm, well defined and measuring on an average 5-30 mm in diameter. Tumor may be seen on the axilla, face, arms, thighs, trunk, scalp and pubic region but the most common site is head [4]. To our knowledge, this is the first case of benign nodular hidradenoma occurring on the lower lip. Case ReportA 77 year old female patient presented our clinic with a mass on her lower lip for three months. Physical examination showed a 3x3 cm, firm, nodular, semi-mobile, pink colored mass on her lower lip (Figure 1).
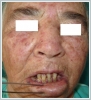
Histopathology report of a previous incisional biopsy performed 15 days ago was reported as pleomorphic adenoma. There was no palpable lymph node on her neck examination. We performed complete removal of tumor from lower lip and repair of tissue defect using Bernard-Burow technique (Figure 2).
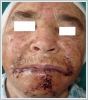
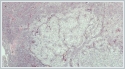
Postoperative histopathological examination of the specimen was reported as benign nodular hidradenoma (Figure 3-4). The patient did not receive any additional treatment. No evidence of recurrence or metastasis occurred during her 4 years of follow-up.
DiscussionDiscussion Nodular hidradenoma also called acrospiroma, clear cell hidradenoma, dermal ductus tumor, hidroacanthoma simplex and poroma is a rare tumor of sweat glands. Clear cell hidradenoma was first reported by Liu in 1949 [5]. Sweat gland tumors are rare neoplasms. They can be classified into benign and malignant variety. The benign forms have been divided into subtypes such as nodular, apocrine and clear cell based on their histopathological presentation. The malignant form or sweat gland carcinomas are those that have an infiltrative and metastatic potential. They are generally classified into two groups. The first group comprises malignant tumors that closely mimic their benign counterparts while tumors in the second group do not have a benign counterpart. Histopathologic features of malignant sweat gland tumors have similarity with malignant salivary gland tumors. “Histopathologic features of malignant sweat gland tumors have similarity with malignant salivary gland tumors. Immunohistochemical analysis of the malignant salivary gland tumors show DNA changes in the form of t(11;19), 39 (q21;p13) translocations resulting in MECT1/MAML2, which differ from sweat gland carcinomas. These changes are similar to that seen in Warthin’s tümör [6]. In our patient histopathology report was pleomorphic adenoma and we did not consider a malignant tumor in our patent. Nodular hidradenoma is a benign tumor but it has a potential risk of neoplastic transformation and metastasis at the same time [7]. The histology of malignant hidradenoma resembles that of its benign counterpart. The criteria for malignancy include poor circumscription, presence of nuclear atypia and mitotic activity, predominantly solid cell islands, infiltrative growth pattern, areas of necrosis and angio-lymphatic permeation [8, 9]. Benign nodular hidradenomas are usually well-shaped and small sized tumors. Malignant nodular hidradenomacarsinomas are separated from benign hidradenomas with their larger sizes and asymmetrical growing patterns. Five year survival for these tumors is low and under 30 % [10]. The average age of incidence for benign hidradenomas is 37.2 years [11]. Malign hidradenomas are aggressive tumors and seen in six to seven decade of the life [12]. They have a local recurrence rate of 50 % and metastasis rate of 60 % [11]. Nodular hidradenoma is called as atypical hidradenoma if there is no evidence of invasion but it has a high mitotic activity or nuclear atypia. The exact frequency of nodular hidradenoma and their risk of transformation into malignant tumors is unknown. However, mitotic activity and cellular pleomorphism may not be accurate predictors of clinical behavior. Malignant hidradenocarcinoma are usually known to arise de novo and malignant transformation of benign nodular hidradenoma has rarely been reported [4]. The main stage of treatment for benign nodular hidradenomas is primary surgical excision of tumor. But the treatment for malign hidradenomas is excision of tumor with a 2 cm tumor free surgical margins and prophylactic neck dissection due to their lymphatic metastasis risk [12]. Conclusions Nodular hidradenomas are benign sweat gland tumors that can be seen anywhere on the body. These tumors are most commonly misdiagnosed as salivary gland tumors due to their histopathological similarities and must be considered in the differential diagnosis. Nodular hidradenomas rarely have local recurrence or malignant transformation and total excision of the tumor is considered as curative. References
Presented atThe manuscript presented as a poster in 34th Turkish National Congress of Otorhinolaryngology Head and Neck Surgery, 10-14 October 2012. Antalya, Turkey. |
|||||||||
| Keywords : hidradenom , dudak , tümör | |||||||||
|